Which White Blood Cellt Ype Has Most Complex Internal Makeup
| Red claret cell | |
|---|---|
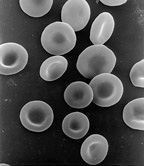 Scanning electron micrograph of human ruby blood cells (ca. 6–viii μm in diameter) | |
| Details | |
| Role | Oxygen transport |
| Identifiers | |
| Acronym(s) | RBC |
| MeSH | D004912 |
| Th | H2.00.04.1.01001 |
| FMA | 62845 |
| Anatomical terms of microanatomy [edit on Wikidata] | |
Carmine claret cells (RBCs), also referred to as cherry-red cells,[ane] red blood corpuscles (in humans or other animals not having nucleus in cherry blood cells), haematids, erythroid cells or erythrocytes (from Greek erythros for "ruby" and kytos for "hollow vessel", with -cyte translated every bit "cell" in modern usage), are the most mutual type of blood cell and the vertebrate's primary means of delivering oxygen (Otwo) to the body tissues—via blood flow through the circulatory system.[two] RBCs accept up oxygen in the lungs, or in fish the gills, and release it into tissues while squeezing through the body's capillaries.
The cytoplasm of a red claret prison cell is rich in hemoglobin, an iron-containing biomolecule that tin bind oxygen and is responsible for the red color of the cells and the blood. Each human being red blood cell contains approximately 270 meg hemoglobin molecules.[3] The cell membrane is equanimous of proteins and lipids, and this structure provides properties essential for physiological cell function such as deformability and stability of the blood cell while traversing the circulatory system and specifically the capillary network.
In humans, mature blood-red blood cells are flexible biconcave disks. They lack a cell nucleus and organelles, to accommodate maximum infinite for hemoglobin; they can exist viewed as sacks of hemoglobin, with a plasma membrane every bit the sack. Approximately 2.4 one thousand thousand new erythrocytes are produced per second in human adults.[4] The cells develop in the bone marrow and broadcast for well-nigh 100–120 days in the body before their components are recycled by macrophages. Each circulation takes nigh sixty seconds (one minute).[5] Approximately 84% of the cells in the human body are 20–30 trillion red blood cells.[half dozen] [7] [8] About half of the claret's book (forty% to 45%) is ruddy blood cells.
Packed ruby-red blood cells (pRBC) are red blood cells that take been donated, candy, and stored in a claret banking company for blood transfusion.
Structure
Vertebrates

There is an immense size variation in vertebrate red blood cells, every bit well every bit a correlation between jail cell and nucleus size. Mammalian ruddy blood cells, which practise not contain nuclei, are considerably smaller than those of nigh other vertebrates.[ix]
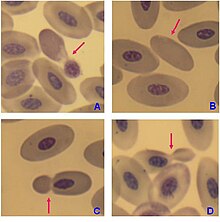
Mature ruby blood cells of birds accept a nucleus, however in the blood of adult females of penguin Pygoscelis papua enucleated scarlet claret cells (B) accept been observed, but with very low frequency.
The vast majority of vertebrates, including mammals and humans, have red blood cells. Red blood cells are cells present in blood to ship oxygen. The only known vertebrates without red claret cells are the crocodile icefish (family Channichthyidae); they live in very oxygen-rich common cold water and transport oxygen freely dissolved in their blood.[10] While they no longer employ hemoglobin, remnants of hemoglobin genes can be found in their genome.[11]
Vertebrate red blood cells consist mainly of hemoglobin, a complex metalloprotein containing heme groups whose iron atoms temporarily bind to oxygen molecules (O2) in the lungs or gills and release them throughout the body. Oxygen can easily diffuse through the cherry blood prison cell'due south cell membrane. Hemoglobin in the carmine blood cells also carries some of the waste product carbon dioxide back from the tissues; most waste carbon dioxide, however, is transported dorsum to the pulmonary capillaries of the lungs as bicarbonate (HCOiii −) dissolved in the blood plasma. Myoglobin, a compound related to hemoglobin, acts to store oxygen in muscle cells.[12]
The color of ruddy blood cells is due to the heme grouping of hemoglobin. The claret plasma lone is harbinger-colored, but the cerise blood cells change color depending on the state of the hemoglobin: when combined with oxygen the resulting oxyhemoglobin is scarlet, and when oxygen has been released the resulting deoxyhemoglobin is of a dark ruby-red burgundy color. However, blood can appear bluish when seen through the vessel wall and peel.[13] Pulse oximetry takes advantage of the hemoglobin color change to directly measure the arterial blood oxygen saturation using colorimetric techniques. Hemoglobin also has a very high affinity for carbon monoxide, forming carboxyhemoglobin which is a very bright scarlet in color. Flushed, confused patients with a saturation reading of 100% on pulse oximetry are sometimes found to be suffering from carbon monoxide poisoning.[ commendation needed ]
Having oxygen-carrying proteins inside specialized cells (as opposed to oxygen carriers being dissolved in torso fluid) was an of import step in the evolution of vertebrates as it allows for less viscous blood, higher concentrations of oxygen, and better diffusion of oxygen from the blood to the tissues. The size of red blood cells varies widely amid vertebrate species; red blood cell width is on boilerplate about 25% larger than capillary diameter, and it has been hypothesized that this improves the oxygen transfer from ruby blood cells to tissues.[14]
Mammals

Typical mammalian crimson claret cells: (a) seen from surface; (b) in profile, forming rouleaux; (c) rendered spherical past h2o; (d) rendered crenate (shrunken and spiky) by salt. (c) and (d) exercise not normally occur in the torso. The last two shapes are due to h2o beingness transported into, and out of, the cells, past osmosis.
The carmine blood cells of mammals are typically shaped every bit biconcave disks: flattened and depressed in the heart, with a dumbbell-shaped cross department, and a torus-shaped rim on the edge of the disk. This shape allows for a high surface-surface area-to-volume (SA/V) ratio to facilitate diffusion of gases.[15] However, there are some exceptions apropos shape in the artiodactyl society (even-toed ungulates including cattle, deer, and their relatives), which displays a broad variety of bizarre red blood jail cell morphologies: small-scale and highly ovaloid cells in llamas and camels (family Camelidae), tiny spherical cells in mouse deer (family Tragulidae), and cells which presume fusiform, lanceolate, crescentic, and irregularly polygonal and other athwart forms in reddish deer and wapiti (family Cervidae). Members of this order have conspicuously evolved a mode of ruby blood cell development substantially unlike from the mammalian norm.[ix] [xvi] Overall, mammalian blood-red blood cells are remarkably flexible and deformable so as to squeeze through tiny capillaries, besides equally to maximize their apposing surface by assuming a cigar shape, where they efficiently release their oxygen load.[17]
Cherry-red blood cells in mammals are unique amongst vertebrates equally they exercise not take nuclei when mature. They practise accept nuclei during early phases of erythropoiesis, but extrude them during development as they mature; this provides more space for hemoglobin. The scarlet blood cells without nuclei, called reticulocytes, subsequently lose all other cellular organelles such equally their mitochondria, Golgi apparatus and endoplasmic reticulum.
The spleen acts as a reservoir of ruddy blood cells, merely this effect is somewhat limited in humans. In some other mammals such equally dogs and horses, the spleen sequesters large numbers of crimson blood cells, which are dumped into the claret during times of exertion stress, yielding a higher oxygen transport capacity.

Scanning electron micrograph of blood cells. From left to correct: human being cherry blood cell, thrombocyte (platelet), leukocyte.
Human being

Two drops of blood are shown with a brilliant red oxygenated drop on the left and a deoxygenated drop on the right.

Blitheness of a typical human red blood prison cell cycle in the circulatory system. This animation occurs at a faster rate (~20 seconds of the average 60-2nd cycle) and shows the carmine claret prison cell deforming as it enters capillaries, as well every bit the bars changing colour as the cell alternates in states of oxygenation along the circulatory system.
A typical human red claret jail cell has a deejay diameter of approximately 6.ii–8.two µm[18] and a thickness at the thickest point of 2–ii.5 µm and a minimum thickness in the centre of 0.8–1 µm, being much smaller than most other human cells. These cells have an average volume of about ninety fL[xix] with a surface expanse of most 136 μm2, and can swell up to a sphere shape containing 150 fL, without membrane distension.
Adult humans have roughly 20–30 trillion ruby blood cells at whatever given time, constituting approximately 70% of all cells by number.[20] Women have well-nigh 4–5 meg cherry-red claret cells per microliter (cubic millimeter) of blood and men nearly 5–6 one thousand thousand; people living at loftier altitudes with low oxygen tension will have more. Red claret cells are thus much more common than the other blood particles: there are about 4,000–11,000 white claret cells and nearly 150,000–400,000 platelets per microliter.
Human ruddy blood cells take on average 60 seconds to consummate one wheel of apportionment.[5] [8] [21]
The blood's ruddy color is due to the spectral backdrop of the hemic iron ions in hemoglobin. Each hemoglobin molecule carries four heme groups; hemoglobin constitutes about a third of the total cell volume. Hemoglobin is responsible for the transport of more than 98% of the oxygen in the torso (the remaining oxygen is carried dissolved in the blood plasma). The cerise blood cells of an average developed homo male shop collectively about 2.5 grams of fe, representing well-nigh 65% of the total iron contained in the trunk.[22] [23]
Microstructure
Nucleus
Carmine blood cells in mammals anucleate when mature, meaning that they lack a jail cell nucleus. In comparison, the red blood cells of other vertebrates have nuclei; the only known exceptions are salamanders of the genus Batrachoseps and fish of the genus Maurolicus.[24] [25]
The elimination of the nucleus in vertebrate ruby-red blood cells has been offered every bit an caption for the subsequent aggregating of non-coding Dna in the genome.[26] The argument runs as follows: Efficient gas transport requires red blood cells to pass through very narrow capillaries, and this constrains their size. In the absence of nuclear elimination, the accumulation of echo sequences is constrained by the volume occupied by the nucleus, which increases with genome size.
Nucleated carmine claret cells in mammals consist of 2 forms: normoblasts, which are normal erythropoietic precursors to mature red blood cells, and megaloblasts, which are abnormally large precursors that occur in megaloblastic anemias.
Membrane limerick
Reddish blood cells are deformable, flexible, are able to attach to other cells, and are able to interface with immune cells. Their membrane plays many roles in this. These functions are highly dependent on the membrane limerick. The cherry-red blood prison cell membrane is composed of 3 layers: the glycocalyx on the outside, which is rich in carbohydrates; the lipid bilayer which contains many transmembrane proteins, as well its lipidic chief constituents; and the membrane skeleton, a structural network of proteins located on the inner surface of the lipid bilayer. Half of the membrane mass in human and most mammalian red blood cells are proteins. The other one-half are lipids, namely phospholipids and cholesterol.[27]
Membrane lipids

The most common red blood cell membrane lipids, schematically disposed as they are distributed on the bilayer. Relative abundances are not at scale.
The scarlet claret cell membrane comprises a typical lipid bilayer, similar to what tin can be found in nearly all human cells. Simply put, this lipid bilayer is composed of cholesterol and phospholipids in equal proportions by weight. The lipid composition is of import as it defines many concrete properties such as membrane permeability and fluidity. Additionally, the activity of many membrane proteins is regulated past interactions with lipids in the bilayer.
Unlike cholesterol, which is evenly distributed between the inner and outer leaflets, the 5 major phospholipids are asymmetrically disposed, as shown beneath:
Outer monolayer
- Phosphatidylcholine (PC);
- Sphingomyelin (SM).
Inner monolayer
- Phosphatidylethanolamine (PE);
- Phosphoinositol (PI) (small amounts).
- Phosphatidylserine (PS);
This asymmetric phospholipid distribution among the bilayer is the consequence of the function of several free energy-dependent and energy-independent phospholipid transport proteins. Proteins called "Flippases" movement phospholipids from the outer to the inner monolayer, while others chosen "floppases" do the contrary operation, against a concentration gradient in an free energy-dependent manner. Additionally, there are also "scramblase" proteins that move phospholipids in both directions at the same fourth dimension, downwards their concentration gradients in an energy-independent manner. There is nevertheless considerable argue ongoing regarding the identity of these membrane maintenance proteins in the red jail cell membrane.
The maintenance of an disproportionate phospholipid distribution in the bilayer (such as an exclusive localization of PS and PIs in the inner monolayer) is disquisitional for the prison cell integrity and office due to several reasons:
- Macrophages recognize and phagocytose cherry cells that expose PS at their outer surface. Thus the confinement of PS in the inner monolayer is essential if the cell is to survive its frequent encounters with macrophages of the reticuloendothelial organisation, specially in the spleen.
- Premature devastation of thallassemic and sickle red cells has been linked to disruptions of lipid asymmetry leading to exposure of PS on the outer monolayer.
- An exposure of PS can potentiate adhesion of cerise cells to vascular endothelial cells, effectively preventing normal transit through the microvasculature. Thus it is of import that PS is maintained only in the inner leaflet of the bilayer to ensure normal claret catamenia in microcirculation.
- Both PS and phosphatidylinositol 4,5-bisphosphate (PIP2) can regulate membrane mechanical function, due to their interactions with skeletal proteins such as spectrin and protein 4.1R. Recent studies accept shown that binding of spectrin to PS promotes membrane mechanical stability. PIP2 enhances the binding of protein ring four.1R to glycophorin C only decreases its interaction with protein band 3, and thereby may attune the linkage of the bilayer to the membrane skeleton.
The presence of specialized structures named "lipid rafts" in the scarlet claret cell membrane have been described by recent studies. These are structures enriched in cholesterol and sphingolipids associated with specific membrane proteins, namely flotillins, STOMatins (band seven), G-proteins, and β-adrenergic receptors. Lipid rafts that have been implicated in cell signaling events in nonerythroid cells have been shown in erythroid cells to mediate β2-adregenic receptor signaling and increase campsite levels, and thus regulating entry of malarial parasites into normal cherry-red cells.[28] [29]
Membrane proteins

The proteins of the membrane skeleton are responsible for the deformability, flexibility and immovability of the red blood prison cell, enabling it to squeeze through capillaries less than half the diameter of the cherry blood cell (7–8 μm) and recovering the discoid shape as soon as these cells end receiving compressive forces, in a similar fashion to an object made of safety.
There are currently more than 50 known membrane proteins, which tin exist in a few hundred up to a one thousand thousand copies per red blood cell. Approximately 25 of these membrane proteins carry the diverse blood group antigens, such equally the A, B and Rh antigens, among many others. These membrane proteins can perform a wide diversity of functions, such as transporting ions and molecules beyond the red cell membrane, adhesion and interaction with other cells such every bit endothelial cells, as signaling receptors, every bit well as other currently unknown functions. The claret types of humans are due to variations in surface glycoproteins of red blood cells. Disorders of the proteins in these membranes are associated with many disorders, such every bit hereditary spherocytosis, hereditary elliptocytosis, hereditary stomatocytosis, and paroxysmal nocturnal hemoglobinuria.[27] [28]
The ruby-red claret cell membrane proteins organized according to their function:

Red blood cell membrane major proteins
Send
- Band 3 – Anion transporter, likewise an of import structural component of the red blood jail cell membrane, makes upwardly to 25% of the jail cell membrane surface, each crimson cell contains approximately ane one thousand thousand copies. Defines the Diego Claret Grouping;[31]
- Aquaporin 1 – h2o transporter, defines the Colton Claret Group;
- Glut1 – glucose and 50-dehydroascorbic acid transporter;
- Kidd antigen poly peptide – urea transporter;
- RHAG – gas transporter, probably of carbon dioxide, defines Rh Blood Group and the associated unusual blood group phenotype Rhnull;
- Na+/K+ – ATPase;
- Catwo+ – ATPase;
- Na+ K+ 2Cl− – cotransporter;
- Na+-Cl− – cotransporter;
- Na-H exchanger;
- Yard-Cl – cotransporter;
- Gardos Aqueduct.
Cell adhesion
- ICAM-4 – interacts with integrins;
- BCAM – a glycoprotein that defines the Lutheran blood group and also known as Lu or laminin-binding protein.
Structural role – The post-obit membrane proteins establish linkages with skeletal proteins and may play an of import role in regulating cohesion between the lipid bilayer and membrane skeleton, likely enabling the red cell to maintain its favorable membrane area by preventing the membrane from collapsing (vesiculating).
- Ankyrin-based macromolecular complex – proteins linking the bilayer to the membrane skeleton through the interaction of their cytoplasmic domains with Ankyrin.
- Band 3 – also assembles various glycolytic enzymes, the presumptive CO2 transporter, and carbonic anhydrase into a macromolecular complex termed a "metabolon," which may play a key role in regulating ruby-red jail cell metabolism and ion and gas transport role.
- RHAG – also involved in send, defines associated unusual blood grouping phenotype Rhmod.
- Protein 4.1R-based macromolecular complex – proteins interacting with Poly peptide 4.1R.
- Protein 4.1R – weak expression of Gerbich antigens;
- Glycophorin C and D – glycoprotein, defines Gerbich Blood Grouping;
- XK – defines the Kell Blood Group and the Mcleod unusual phenotype (lack of Kx antigen and greatly reduced expression of Kell antigens);
- RhD/RhCE – defines Rh Blood Grouping and the associated unusual claret grouping phenotype Rhnil;
- Duffy protein – has been proposed to be associated with chemokine clearance;[32]
- Adducin – interaction with band iii;
- Dematin- interaction with the Glut1 glucose transporter.
[27] [28]
Surface electrostatic potential
The zeta potential is an electrochemical belongings of cell surfaces that is determined by the net electrical charge of molecules exposed at the surface of cell membranes of the cell. The normal zeta potential of the red claret prison cell is −15.7 millivolts (mV).[33] Much of this potential appears to exist contributed by the exposed sialic acid residues in the membrane: their removal results in zeta potential of −6.06 mV.
Function
Role in CO2 transport
Recall that respiration, equally illustrated schematically hither with a unit of measurement of carbohydrate, produces near every bit many molecules of carbon dioxide, CO2, as information technology consumes of oxygen, Otwo.[34]
Thus, the office of the circulatory organisation is as much nigh the transport of carbon dioxide every bit nearly the transport of oxygen. As stated elsewhere in this commodity, well-nigh of the carbon dioxide in the claret is in the form of bicarbonate ion. The bicarbonate provides a critical pH buffer.[35] Thus, different hemoglobin for Otwo send, there is a physiological advantage to not having a specific CO2 transporter molecule.
Red blood cells, still, play a primal role in the CO2 transport process, for two reasons. Get-go, considering, besides hemoglobin, they contain a large number of copies of the enzyme carbonic anhydrase on the inside of their cell membrane.[36] Carbonic anhydrase, as its name suggests, acts as a catalyst of the exchange betwixt carbonic acid and carbon dioxide (which is the anhydride of carbonic acid). Because it is a goad, it tin bear upon many CO2 molecules, and then it performs its essential role without needing as many copies every bit are needed for Oii transport by hemoglobin. In the presence of this catalyst carbon dioxide and carbonic acrid attain an equilibrium very rapidly, while the ruddy cells are however moving through the capillary. Thus it is the RBC that ensures that well-nigh of the CO2 is transported as bicarbonate.[37] [38] At physiological pH the equilibrium strongly favors carbonic acid, which is by and large dissociated into bicarbonate ion.[39]
The H+ ions released by this rapid reaction within RBC, while still in the capillary, act to reduce the oxygen binding affinity of hemoglobin, the Bohr result.
The second major contribution of RBC to carbon dioxide send is that carbon dioxide directly reacts with globin protein components of hemoglobin to form carbaminohemoglobin compounds. Every bit oxygen is released in the tissues, more CO2 binds to hemoglobin, and as oxygen binds in the lung, it displaces the hemoglobin bound COii, this is called the Haldane effect. Despite the fact that only a minor amount of the CO2 in blood is leap to hemoglobin in venous blood, a greater proportion of the alter in CO2 content between venous and arterial blood comes from the change in this bound CO2.[40] That is, there is always an abundance of bicarbonate in claret, both venous and arterial, because of its aforementioned role as a pH buffer.
In summary, carbon dioxide produced by cellular respiration diffuses very rapidly to areas of lower concentration, specifically into nearby capillaries.[41] [42] When it diffuses into a RBC, CO2 is chop-chop converted by the carbonic anhydrase found on the inside of the RBC membrane into bicarbonate ion. The bicarbonate ions in turn leave the RBC in exchange for chloride ions from the plasma, facilitated by the band 3 anion transport poly peptide colocated in the RBC membrane. The bicarbonate ion does not lengthened back out of the capillary, just is carried to the lung. In the lung the lower partial pressure of carbon dioxide in the alveoli causes carbon dioxide to diffuse chop-chop from the capillary into the alveoli. The carbonic anhydrase in the ruby-red cells keeps the bicarbonate ion in equilibrium with carbon dioxide. So as carbon dioxide leaves the capillary, and COtwo is displaced by Otwo on hemoglobin, sufficient bicarbonate ion converts rapidly to carbon dioxide to maintain the equilibrium.[36] [43] [44] [45]
Secondary functions
When red claret cells undergo shear stress in constricted vessels, they release ATP, which causes the vessel walls to relax and dilate so as to promote normal blood menstruum.[46]
When their hemoglobin molecules are deoxygenated, cerise blood cells release S-Nitrosothiols, which also act to dilate blood vessels,[47] thus directing more blood to areas of the body depleted of oxygen.
Red claret cells can also synthesize nitric oxide enzymatically, using Fifty-arginine every bit substrate, equally do endothelial cells.[48] Exposure of carmine claret cells to physiological levels of shear stress activates nitric oxide synthase and export of nitric oxide,[49] which may contribute to the regulation of vascular tonus.
Red blood cells tin can as well produce hydrogen sulfide, a signalling gas that acts to relax vessel walls. It is believed that the cardioprotective effects of garlic are due to crimson blood cells converting its sulfur compounds into hydrogen sulfide.[50]
Red blood cells likewise play a part in the trunk'south immune response: when lysed by pathogens such as bacteria, their hemoglobin releases free radicals, which interruption down the pathogen'southward prison cell wall and membrane, killing it.[51] [52]
Cellular processes
As a result of not containing mitochondria, red claret cells employ none of the oxygen they ship; instead they produce the energy carrier ATP by the glycolysis of glucose and lactic acid fermentation on the resulting pyruvate.[53] [54] Furthermore, the pentose phosphate pathway plays an important function in carmine blood cells; see glucose-half dozen-phosphate dehydrogenase deficiency for more information.
As red blood cells contain no nucleus, poly peptide biosynthesis is currently assumed to be absent in these cells.
Considering of the lack of nuclei and organelles, mature red blood cells practise not contain DNA and cannot synthesize any RNA, and consequently cannot split and take express repair capabilities.[55] The disability to carry out poly peptide synthesis means that no virus can evolve to target mammalian red blood cells.[56] However, infection with parvoviruses (such as human parvovirus B19) can affect erythroid precursors while they nevertheless have Dna, as recognized by the presence of giant pronormoblasts with viral particles and inclusion bodies, thus temporarily depleting the claret of reticulocytes and causing anemia.[57]
Life cycle
Homo red blood cells are produced through a process named erythropoiesis, developing from committed stalk cells to mature ruby claret cells in about 7 days. When matured, in a healthy individual these cells live in blood circulation for nearly 100 to 120 days (and 80 to 90 days in a total term baby).[58] At the finish of their lifespan, they are removed from apportionment. In many chronic diseases, the lifespan of the red blood cells is reduced.
Creation
Erythropoiesis is the procedure past which new crimson blood cells are produced; it lasts virtually 7 days. Through this process red blood cells are continuously produced in the red bone marrow of large bones. (In the embryo, the liver is the master site of cherry blood cell production.) The production tin can exist stimulated by the hormone erythropoietin (EPO), synthesised past the kidney. Only earlier and afterwards leaving the bone marrow, the developing cells are known equally reticulocytes; these constitute nearly 1% of circulating red claret cells.
Functional lifetime
The functional lifetime of a ruddy blood cell is near 100–120 days, during which time the carmine blood cells are continually moved by the blood menstruation push (in arteries), pull (in veins) and a combination of the two equally they squeeze through microvessels such as capillaries. They are also recycled in the bone marrow.[59]
Senescence
The crumbling cherry-red blood cell undergoes changes in its plasma membrane, making it susceptible to selective recognition by macrophages and subsequent phagocytosis in the mononuclear phagocyte system (spleen, liver and lymph nodes), thus removing old and lacking cells and continually purging the claret. This process is termed eryptosis, red blood cell programmed death.[lx] This process commonly occurs at the aforementioned rate of production past erythropoiesis, balancing the full circulating red blood prison cell count. Eryptosis is increased in a wide multifariousness of diseases including sepsis, haemolytic uremic syndrome, malaria, sickle cell anemia, beta-thalassemia, glucose-6-phosphate dehydrogenase deficiency, phosphate depletion, fe deficiency and Wilson's illness. Eryptosis can be elicited by osmotic shock, oxidative stress, and free energy depletion, likewise as by a wide variety of endogenous mediators and xenobiotics. Excessive eryptosis is observed in red blood cells lacking the cGMP-dependent protein kinase type I or the AMP-activated protein kinase AMPK. Inhibitors of eryptosis include erythropoietin, nitric oxide, catecholamines and high concentrations of urea.
Much of the resulting breakdown products are recirculated in the body. The heme constituent of hemoglobin are broken down into atomic number 26 (Atomic number 26iii+) and biliverdin. The biliverdin is reduced to bilirubin, which is released into the plasma and recirculated to the liver bound to albumin. The atomic number 26 is released into the plasma to be recirculated by a carrier protein called transferrin. Nigh all red claret cells are removed in this manner from the circulation before they are former enough to hemolyze. Hemolyzed hemoglobin is leap to a protein in plasma chosen haptoglobin, which is non excreted by the kidney.[61]
Clinical significance
Affliction
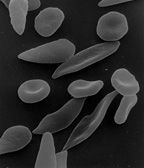
Affected by Sickle-cell disease, red blood cells alter shape and threaten to damage internal organs.
Blood diseases involving the red blood cells include:
- Anemias (or anaemias) are diseases characterized by depression oxygen transport capacity of the blood, because of low red cell count or some abnormality of the red blood cells or the hemoglobin.
-
- Fe deficiency anemia is the nearly common anemia; it occurs when the dietary intake or assimilation of iron is insufficient, and hemoglobin, which contains iron, cannot exist formed
-
- Sickle-cell affliction is a genetic affliction that results in abnormal hemoglobin molecules. When these release their oxygen load in the tissues, they go insoluble, leading to mis-shaped red claret cells. These sickle shaped scarlet cells are less deformable and viscoelastic, meaning that they have become rigid and tin cause blood vessel blockage, pain, strokes, and other tissue impairment.
-
- Thalassemia is a genetic illness that results in the production of an abnormal ratio of hemoglobin subunits.
-
- Hereditary spherocytosis syndromes are a group of inherited disorders characterized past defects in the scarlet blood cell'southward cell membrane, causing the cells to be pocket-sized, sphere-shaped, and delicate instead of donut-shaped and flexible. These abnormal cherry blood cells are destroyed past the spleen. Several other hereditary disorders of the red blood cell membrane are known.[62]
-
- Pernicious anemia is an autoimmune affliction wherein the body lacks intrinsic cistron, required to absorb vitamin B12 from nutrient. Vitamin B12 is needed for the product of hemoglobin.
-
- Aplastic anemia is caused by the inability of the os marrow to produce blood cells.
-
- Pure reddish cell aplasia is caused by the inability of the os marrow to produce only ruddy blood cells.
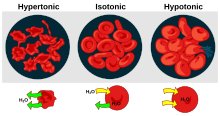

Micrographs of the effects of osmotic pressure
- Hemolysis is the general term for excessive breakdown of red blood cells. Information technology can take several causes and can result in hemolytic anemia.
-
- The malaria parasite spends part of its life-wheel in scarlet blood cells, feeds on their hemoglobin then breaks them apart, causing fever. Both sickle-prison cell illness and thalassemia are more mutual in malaria areas, because these mutations convey some protection against the parasite.
- Polycythemias (or erythrocytoses) are diseases characterized by a surplus of red blood cells. The increased viscosity of the blood tin can cause a number of symptoms.
-
- In polycythemia vera the increased number of ruddy blood cells results from an abnormality in the bone marrow.
- Several microangiopathic diseases, including disseminated intravascular coagulation and thrombotic microangiopathies, present with pathognomonic (diagnostic) red blood cell fragments called schistocytes. These pathologies generate fibrin strands that sever blood-red blood cells as they try to motion by a thrombus.
Transfusion
Red blood cells may be given every bit part of a blood transfusion. Blood may be donated from some other person, or stored by the recipient at an earlier date. Donated blood commonly requires screening to ensure that donors practise not contain risk factors for the presence of claret-borne diseases, or will non endure themselves by giving claret. Claret is usually collected and tested for common or serious claret-borne diseases including Hepatitis B, Hepatitis C and HIV. The blood blazon (A, B, AB, or O) or the blood production is identified and matched with the recipient's blood to minimise the likelihood of acute hemolytic transfusion reaction, a blazon of transfusion reaction. This relates to the presence of antigens on the cell's surface. Later on this process, the blood is stored, and within a brusque elapsing is used. Blood can exist given as a whole product or the red blood cells separated as packed cherry-red blood cells.
Blood is often transfused when there is known anaemia, active bleeding, or when there is an expectation of serious claret loss, such as prior to an operation. Earlier claret is given, a modest sample of the recipient's blood is tested with the transfusion in a procedure known every bit cross-matching.
In 2008 it was reported that homo embryonic stem cells had been successfully coaxed into becoming ruby-red blood cells in the lab. The difficult footstep was to induce the cells to squirt their nucleus; this was accomplished by growing the cells on stromal cells from the bone marrow. Information technology is hoped that these artificial red claret cells can eventually be used for claret transfusions.[63]
Tests
Several claret tests involve crimson blood cells. These include a RBC count (the number of red claret cells per book of blood), calculation of the hematocrit (percent of blood volume occupied by red blood cells), and the erythrocyte sedimentation rate. The blood type needs to exist determined to prepare for a claret transfusion or an organ transplantation.
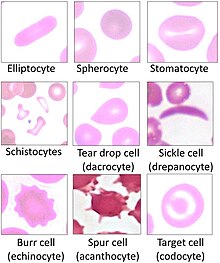
Many diseases involving carmine blood cells are diagnosed with a blood film (or peripheral blood smear), where a thin layer of blood is smeared on a microscope slide. This may reveal poikilocytosis, which are variations in red claret jail cell shape. When red blood cells sometimes occur as a stack, flat side adjacent to flat side. This is known as rouleaux germination, and it occurs more than often if the levels of certain serum proteins are elevated, as for instance during inflammation.
Separation and claret doping
Cerise claret cells can be obtained from whole blood past centrifugation, which separates the cells from the claret plasma in a process known as claret fractionation. Packed ruby-red blood cells, which are made in this way from whole claret with the plasma removed, are used in transfusion medicine.[64] During plasma donation, the red blood cells are pumped back into the trunk right away and just the plasma is collected.
Some athletes have tried to improve their functioning past blood doping: first about 1 litre of their blood is extracted, so the red blood cells are isolated, frozen and stored, to be reinjected shortly earlier the competition. (Red claret cells can exist conserved for 5 weeks at −79 °C or −110 °F, or over x years using cryoprotectants[65]) This practice is hard to detect just may endanger the human cardiovascular system which is not equipped to deal with claret of the resulting higher viscosity. Another method of blood doping involves injection with erythropoietin to stimulate production of cerise blood cells. Both practices are banned past the Earth Anti-Doping Bureau.
History
The first person to describe red blood cells was the immature Dutch biologist Jan Swammerdam, who had used an early microscope in 1658 to report the blood of a frog.[66] Unaware of this work, Anton van Leeuwenhoek provided another microscopic clarification in 1674, this time providing a more precise description of red blood cells, fifty-fifty approximating their size, "25,000 times smaller than a fine grain of sand".
In the 1740s, Vincenzo Menghini in Bologna was able to demonstrate the presence of iron past passing magnets over the pulverization or ash remaining from heated cherry-red blood cells.
In 1901, Karl Landsteiner published his discovery of the three main claret groups—A, B, and C (which he later renamed to O). Landsteiner described the regular patterns in which reactions occurred when serum was mixed with ruby claret cells, thus identifying uniform and conflicting combinations between these blood groups. A twelvemonth later Alfred von Decastello and Adriano Sturli, two colleagues of Landsteiner, identified a fourth blood group—AB.
In 1959, by employ of 10-ray crystallography, Dr. Max Perutz was able to unravel the structure of hemoglobin, the ruby-red blood cell protein that carries oxygen.[67]
The oldest intact carmine claret cells always discovered were establish in Ötzi the Iceman, a natural mummy of a man who died around 3255 BCE. These cells were discovered in May 2012.[68]
See also
- Altitude grooming
- Claret substitute
- Red blood cell indices
- Serum (blood)
- Er claret group collection
References
- ^ Vinay Kumar; Abul Grand. Abbas; Nelson Fausto; Richard N. Mitchell (2007). Robbins Basic Pathology (8th ed.). Saunders.
- ^ "Blood Cells". Archived from the original on 23 July 2016.
- ^ D'Alessandro, Angelo (2017). "Red blood jail cell proteomics update: is in that location more to discover?". Blood Transfusion. 15 (2): 182–87. doi:ten.2450/2017.0293-16. PMC5336341. PMID 28263177.
- ^ Erich Sackmann, Biological Membranes Compages and Function., Handbook of Biological Physics, (ed. R.Lipowsky and Eastward.Sackmann, vol.1, Elsevier, 1995
- ^ a b J. A. Blom (2003). Monitoring of Respiration and Apportionment. CRC Press. p. 27. ISBN978-0-203-50328-7.
- ^ Sender, Ron; Fuchs, Shai; Milo, Ron (19 August 2016). "Revised Estimates for the Number of Human being and Bacteria Cells in the Body". PLOS Biology. 14 (8): e1002533. doi:ten.1371/journal.pbio.1002533. PMC4991899. PMID 27541692.
- ^ Laura Dean. Claret Groups and Red Jail cell Antigens
- ^ a b Pierigè F, Serafini Due south, Rossi L, Magnani M (January 2008). "Cell-based drug delivery". Advanced Drug Commitment Reviews. 60 (2): 286–95. doi:ten.1016/j.addr.2007.08.029. PMID 17997501.
{{cite journal}}: CS1 maint: uses authors parameter (link) - ^ a b Gulliver, Yard. (1875). "On the size and shape of red corpuscles of the claret of vertebrates, with drawings of them to a uniform scale, and extended and revised tables of measurements". Proceedings of the Zoological Society of London. 1875: 474–95.
- ^ Ruud JT (May 1954). "Vertebrates without erythrocytes and blood pigment". Nature. 173 (4410): 848–50. Bibcode:1954Natur.173..848R. doi:ten.1038/173848a0. PMID 13165664. S2CID 3261779.
- ^ Carroll, Sean (2006). The Making of the Fittest. Due west.Due west. Norton. ISBN978-0-393-06163-5.
- ^ Maton, Anthea; Jean Hopkins; Charles William McLaughlin; Susan Johnson; Maryanna Quon Warner; David LaHart; Jill D. Wright (1993). Human being Biology and Health . Englewood Cliffs, New Jersey: Prentice Hall. ISBN978-0-thirteen-981176-0.
- ^ Anthis, Nick (17 April 2008). "Why Are Veins Blue?". Scienceblogs . Retrieved 23 Apr 2015.
- ^ Snyder, Gregory K.; Sheafor, Brandon A. (1999). "Red Blood Cells: Centerpiece in the Development of the Vertebrate Circulatory System". Integrative and Comparative Biology. 39 (2): 189. doi:x.1093/icb/39.2.189.
- ^ "BBC Bitesize – GCSE Biology – Blood – Revision 2". www.bbc.co.united kingdom . Retrieved 26 November 2017.
- ^ Gregory TR (2001). "The bigger the C-value, the larger the prison cell: genome size and reddish claret cell size in vertebrates". Blood Cells, Molecules & Diseases. 27 (5): 830–43. CiteSeerX10.ane.1.22.9555. doi:10.1006/bcmd.2001.0457. PMID 11783946.
- ^ Goodman SR, Kurdia A, Ammann L, Kakhniashvili D, Daescu O (December 2007). "The human cherry-red claret cell proteome and interactome". Experimental Biology and Medicine. 232 (11): 1391–408. doi:10.3181/0706-MR-156. PMID 18040063. S2CID 32326166.
{{cite journal}}: CS1 maint: uses authors parameter (link) - ^ Mary Louise Turgeon (2004). Clinical Hematology: Theory and Procedures. Lippincott Williams & Wilkins. p. 100. ISBN9780781750073.
- ^ McLaren CE, Brittenham GM, Hasselblad V (April 1987). "Statistical and graphical evaluation of erythrocyte book distributions". Am. J. Physiol. 252 (iv Pt two): H857–66. CiteSeerX10.1.one.1000.348. doi:x.1152/ajpheart.1987.252.four.H857. PMID 3565597.
{{cite periodical}}: CS1 maint: uses authors parameter (link) - ^ Bianconi, Eva; Piovesan, Allison; Facchin, Federica; Beraudi, Alina; Casadei, Raffaella; Frabetti, Flavia; Vitale, Lorenza; Pelleri, Maria Chiara; Tassani, Simone (i November 2013). "An estimation of the number of cells in the human being body". Annals of Human Biology. 40 (6): 463–71. doi:x.3109/03014460.2013.807878. ISSN 0301-4460. PMID 23829164. S2CID 16247166.
- ^ Hillman, Robert S.; Ault, Kenneth A.; Rinder, Henry M. (2005). Hematology in Clinical Practice: A Guide to Diagnosis and Management (4 ed.). McGraw-Hill Professional. p. 1. ISBN978-0-07-144035-half dozen.
- ^ Iron Metabolism, University of Virginia Pathology. Accessed 22 September 2007.
- ^ Iron Transport and Cellular Uptake by Kenneth R. Bridges, Information Center for Sickle Cell and Thalassemic Disorders. Accessed 22 September 2007.
- ^ Cohen, West. D. (1982). "The cytomorphic organisation of anucleate non-mammalian erythrocytes". Protoplasma. 113: 23–32. doi:10.1007/BF01283036. S2CID 41287948.
- ^ Wingstrand KG (1956). "Non-nucleated erythrocytes in a teleostean fish Maurolicus mülleri (Gmelin)". Zeitschrift für Zellforschung und Mikroskopische Anatomie. 45 (2): 195–200. doi:10.1007/BF00338830. PMID 13402080. S2CID 12916049.
- ^ Gregory, T. R. (2001). "The Bigger the C-Value, the Larger the Cell: Genome Size and Carmine Claret Cell Size in Vertebrates". Blood Cells, Molecules and Diseases. 27 (five): 830–43. CiteSeerX10.i.one.22.9555. doi:x.1006/bcmd.2001.0457. PMID 11783946.
- ^ a b c Yazdanbakhsh Chiliad, Lomas-Francis C, Reid ME (October 2000). "Blood groups and diseases associated with inherited abnormalities of the ruddy blood cell membrane". Transfusion Medicine Reviews. fourteen (four): 364–74. doi:10.1053/tmrv.2000.16232. PMID 11055079.
{{cite periodical}}: CS1 maint: uses authors parameter (link) - ^ a b c Mohandas N, Gallagher PG (Nov 2008). "Ruddy cell membrane: past, nowadays, and future". Blood. 112 (ten): 3939–48. doi:10.1182/blood-2008-07-161166. PMC2582001. PMID 18988878.
{{cite journal}}: CS1 maint: uses authors parameter (link) - ^ Rodi PM, Trucco VM, Gennaro AM (June 2008). "Factors determining detergent resistance of erythrocyte membranes". Biophysical Chemistry. 135 (1–3): 14–18. doi:x.1016/j.bpc.2008.02.015. PMID 18394774.
{{cite periodical}}: CS1 maint: uses authors parameter (link) - ^ Hempelmann Eastward, Götze O (1984). "Characterization of membrane proteins by polychromatic silverish staining". Hoppe-Seyler'south Z Physiol Chem. 365: 241–42.
- ^ Iolascon A, Perrotta South, Stewart GW (March 2003). "Cherry blood prison cell membrane defects". Reviews in Clinical and Experimental Hematology. 7 (ane): 22–56. PMID 14692233.
{{cite journal}}: CS1 maint: uses authors parameter (link) - ^ Denomme GA (July 2004). "The structure and function of the molecules that carry human red blood prison cell and platelet antigens". Transfusion Medicine Reviews. 18 (iii): 203–31. doi:10.1016/j.tmrv.2004.03.006. PMID 15248170.
- ^ Tokumasu F, Ostera GR, Amaratunga C, Fairhurst RM (2012) Modifications in erythrocyte membrane zeta potential past Plasmodium falciparum infection. Exp Parasitol
- ^ Guyton, Arthur C., M.D. (1976). "Ch. 41 Transport of Oxygen and Carbon Dioxide in the Blood and Body Fluids". Textbook of Medical Physiology (5th ed.). Philadelphia, PA: Westward. B. Saunders. p. 556. ISBN0-7216-4393-0.
The Respiratory Exchange Ratio is 1:one when carbohydrate is consumed, it is equally low as 0.seven when fatty is consumed.
- ^ West, John B., G.D., PhD (1974). "Gas Ship to the Periphery". Respiratory Physiology – the essentials. Baltimore, MD: Williams & Wilkens. p. 80. ISBN0-683-08932-3.
Acid Base Status: The transport of CO2 has a profound effect on the acid-base status of claret and the body as a whole. The lung excretes over 10,000 mEq of carbonic acrid per day compared to less than 100 mEq of fixed acids by the kidney.
- ^ a b Guyton, Arthur C., Grand.D. (1976). "Ch. 41 Transport of Oxygen and Carbon Dioxide in the Blood and Body Fluids". Textbook of Medical Physiology (Fifth ed.). Philadelphia, PA: W. B. Saunders. pp. 553–554. ISBN0-7216-4393-0.
Reaction of Carbon Dioxide with Water in the Scarlet Blood Cells - Effect of Carbonic Anhydrase
- ^ Guyton, Arthur C., Thousand.D. (1976). "Ch. 41 Transport of Oxygen and Carbon Dioxide in the Blood and Body Fluids". Textbook of Medical Physiology (Fifth ed.). Philadelphia, PA: W. B. Saunders. pp. 553–554. ISBN0-7216-4393-0.
carbonic anhydrase catalyzes the reaction betwixt carbon dioxide and water.
- ^ Comroe, Julius H, Jr, M.D. (1965). "Transport and emptying of carbon dioxide". Physiology of Respiration (1971 ed.). Chicago, IL: Year Volume Medical Publishers. p. 176. ISBN0-8151-1824-4.
[carbonic anhdrase] makes the reaction become to the right about 13000 times every bit fast
- ^ Diem, G.; Lentner, C., eds. (1970). "Blood Gasses". Documenta Geigy Scientific Tables (seventh ed.). Basle, Switzerland: Ciba-Geigy Limited. pp. 570–571.
In plasma about 5% of CO2 is in physical solution 94% as bicarbonate and one% as carbamino compounds; in the erythrocytes the corresponding figures are 7%, 82% and 11%.
- ^ Guyton, Arthur C., M.D. (1976). "Ch. 41 Ship of Oxygen and Carbon Dioxide in the Blood and Body Fluids". Textbook of Medical Physiology (5th ed.). Philadelphia, PA: W. B. Saunders. p. 554. ISBN0-7216-4393-0.
from figure 41-5 Hgb.CO2 is about 23% and bicarbonate is about 70% of the total carbon dioxide transported to the lungs.
- ^ Comroe, Julius H, Jr, M.D. (1965). "Pulmonary Gas Diffusion". Physiology of Respiration (1971 ed.). Chicago, IL: Yr Book Medical Publishers. p. 140. ISBN0-8151-1824-iv.
Despite being a heavier molecule, because it is more soluble, the relative rate of diffusion of CO2 is about 20 times the rate of O2
- ^ Guyton, Arthur C., Chiliad.D. (1976). "Ch. 41 Transport of Oxygen and Carbon Dioxide in the Blood and Body Fluids". Textbook of Medical Physiology (Fifth ed.). Philadelphia, PA: W. B. Saunders. p. 553. ISBN0-7216-4393-0.
carbon dioxide diffuses out of the tissue cells in the gaseous form (only not to a meaning effect in the bicarbonate class considering the cell membrane is far less permeable to bicarbonate than to the dissolved gas.
- ^ Comroe, Julius H, Jr, K.D. (1965). "Transport and elimination of carbon dioxide". Physiology of Respiration (1971 ed.). Chicago, IL: Yr Book Medical Publishers. pp. 175–177. ISBN0-8151-1824-4.
the buffering occurred in the red cell
- ^ West, John B., M.D., PhD (1974). "Gas Transport to the Periphery". Respiratory Physiology – the essentials. Baltimore, Dr.: Williams & Wilkens. pp. 77–79. ISBN0-683-08932-three.
CO2 Transport
- ^ William E. Stone, PhD (1973). "Ch. 6-1 Uptake and Delivery of the Respiratory Gasses". In Brobeck, John R., PhD, M.D. (ed.). Best & Taylor'southward Physiological basis of medical practice (9th ed.). Baltimore, Physician: Williams & Wilkins. pp. 6.16–6.18. ISBN0-683-10160-9.
Transport of CO2 as Bicarbonate
- ^ Wan J, Ristenpart WD, Stone HA (October 2008). "Dynamics of shear-induced ATP release from red blood cells". Proceedings of the National Academy of Sciences of the Usa. 105 (43): 16432–vii. Bibcode:2008PNAS..10516432W. doi:10.1073/pnas.0805779105. PMC2575437. PMID 18922780.
{{cite journal}}: CS1 maint: uses authors parameter (link) - ^ Diesen DL, Hess DT, Stamler JS (August 2008). "Hypoxic vasodilation by red claret cells: evidence for an s-nitrosothiol-based signal". Circulation Research. 103 (v): 545–53. doi:x.1161/CIRCRESAHA.108.176867. PMC2763414. PMID 18658051.
{{cite periodical}}: CS1 maint: uses authors parameter (link) - ^ Kleinbongard P, Schutz R, Rassaf T, et al. (2006). "Red blood cells limited a functional endothelial nitric oxide synthase". Blood. 107 (7): 2943–51. doi:10.1182/claret-2005-x-3992. PMID 16368881.
- ^ Ulker P, Sati 50, Celik-Ozenci C, Meiselman HJ, Baskurt OK (2009). "Mechanical stimulation of nitric oxide synthesizing mechanisms in erythrocytes". Biorheology. 46 (2): 121–32. doi:ten.3233/BIR-2009-0532. PMID 19458415.
{{cite journal}}: CS1 maint: uses authors parameter (link) - ^ Benavides, Gloria A; Victor 1000 Darley-Usmar; Mills, R. West.; Patel, H. D.; Isbell, T. S.; Patel, R. P.; Darley-Usmar, V. M.; Doeller, J. E.; Kraus, D. W. (xiii November 2007). "Hydrogen sulfide mediates the vasoactivity of garlic". Proceedings of the National Academy of Sciences of the U.s.a. of America. 104 (46): 17977–17982. Bibcode:2007PNAS..10417977B. doi:10.1073/pnas.0705710104. PMC2084282. PMID 17951430.
- ^ Kesava, Shobana (1 September 2007). "Red claret cells do more than simply carry oxygen; New findings by NUS team show they aggressively set on bacteria likewise" (PDF). The Straits Times . Retrieved 26 March 2013.
- ^ Jiang Northward, Tan NS, Ho B, Ding JL (Oct 2007). "Respiratory protein-generated reactive oxygen species as an antimicrobial strategy". Nature Immunology. viii (10): 1114–22. doi:10.1038/ni1501. PMID 17721536. S2CID 11359246.
{{cite journal}}: CS1 maint: uses authors parameter (link) - ^ Jr, Jeremy Thousand. Berg, John L. Tymoczko, Lubert Stryer; with Gregory J. Gatto (2012). Biochemistry (seventh ed.). New York: Due west.H. Freeman. pp. 455, 609. ISBN9781429229364.
- ^ Tilton, WM; Seaman, C; Carriero, D; Piomelli, South (August 1991). "Regulation of glycolysis in the erythrocyte: part of the lactate/pyruvate and NAD/NADH ratios". The Periodical of Laboratory and Clinical Medicine. 118 (2): 146–52. PMID 1856577.
- ^ Kabanova South, Kleinbongard P, Volkmer J, Andrée B, Kelm Grand, Jax TW (2009). "Gene expression assay of human ruby-red claret cells". International Journal of Medical Sciences. 6 (four): 156–nine. doi:10.7150/ijms.6.156. PMC2677714. PMID 19421340.
{{cite periodical}}: CS1 maint: uses authors parameter (link) - ^ Zimmer, Carl (27 March 2007). "Scientists Explore Ways to Lure Viruses to Their Death". The New York Times . Retrieved 26 March 2013.
- ^ Erik D. Heegaard & Kevin E. Brown (July 2002). "Homo parvovirus B19". Clin Microbiol Rev. 15 (3): 485–505. doi:10.1128/CMR.fifteen.3.485-505.2002. PMC118081. PMID 12097253.
- ^ Harrison, K. 50. (1979). "Fetal Erythrocyte Lifespan". Journal of Paediatrics and Child Wellness. 15 (2): 96–97. doi:10.1111/j.1440-1754.1979.tb01197.10. PMID 485998. S2CID 5370064.
- ^ Higgins, John (2014). "Red Blood Prison cell Population Dynamics". Clinics in Laboratory Medicine. 35 (i): 43–57. doi:ten.1016/j.cll.2014.10.002. PMC4717490. PMID 25676371.
- ^ Lang F, Lang Due east, Föller Yard (2012). "Physiology and pathophysiology of eryptosis". Transfusion Medicine and Hemotherapy. 39 (5): 308–14. doi:10.1159/000342534. PMC3678267. PMID 23801921.
{{cite periodical}}: CS1 maint: uses authors parameter (link) - ^ Föller M, Huber SM, Lang F (October 2008). "Erythrocyte programmed cell death". IUBMB Life. lx (10): 661–68. doi:x.1002/iub.106. PMID 18720418. S2CID 41603762.
{{cite journal}}: CS1 maint: uses authors parameter (link) - ^ An X, Mohandas N (May 2008). "Disorders of reddish cell membrane". British Journal of Haematology. 141 (3): 367–75. doi:10.1111/j.1365-2141.2008.07091.ten. PMID 18341630. S2CID 7313716.
{{cite journal}}: CS1 maint: uses authors parameter (link) - ^ Commencement ruddy blood cells grown in the lab, New Scientist News, 19 August 2008
- ^ "Circular of Data for Blood and Blood Products" (PDF). American Association of Claret Banks, American Red Cantankerous, America's Blood Centers. Archived from the original (PDF) on thirty Oct 2011. Retrieved ane November 2010.
- ^ Sparacino, Linette; Manning, Frederick J.; Availability, Constitute of Medicine (US) Forum on Claret Safety and Blood (eight February 1996). Frozen Ruddy Cell Engineering. National Academies Press (United states of america) – via www.ncbi.nlm.nih.gov.
- ^ "Swammerdam, Jan (1637–1680)", McGraw Hill AccessScience, 2007. Accessed 27 December 2007.
- ^ "Max F. Perutz – Biographical". NobelPrize.org . Retrieved 23 October 2018.
- ^ Stephanie Pappas (2 May 2012). "'Iceman' mummy holds world's oldest claret cells". Fox News . Retrieved two May 2012.
External links
- Blood Groups and Red Prison cell Antigens by Laura Dean. Searchable and downloadable online textbook in the public domain.
- Database of vertebrate erythrocyte sizes.
- Ruddy Gold, PBS site containing facts and history
Which White Blood Cellt Ype Has Most Complex Internal Makeup,
Source: https://en.wikipedia.org/wiki/Red_blood_cell
Posted by: carrdidellp.blogspot.com




0 Response to "Which White Blood Cellt Ype Has Most Complex Internal Makeup"
Post a Comment